Meniscal Problems
If you have further questions about meniscal problems then please feel free to contact us
here.
Alternatively you can book an appointment to see us below.
The meniscus is a C-shaped piece of cartilage that sits between the femur (thigh bone) and the tibia (shin bone) and is attached to the lining of the knee joint. There are two menisci in a normal knee; the one on the inner side of the knee is called the medial meniscus and the one on the outer side of the knee is called the lateral meniscus. The menisci act as shock absorbers within the knee joint, protecting the articular cartilage (gristle) that lines the surface of the bone from impact. They also have a stabilising role and cup the femur preventing excessive movement of the femur on the tibia.
Menisci are a commonly damaged knee structure. The injury may occur in any age group, however in younger people where the meniscus is tough and rubbery it may take a forceful twisting injury to do so (figure 1). In older people, where the meniscus is often degenerate and weak, it may only require a trivial mechanism to tear (such as squatting).
There are two different mechanisms for tearing a meniscus.
Traumatic tears result from a sudden load being applied to the meniscus that is severe enough to cause the meniscal cartilage to fail and separate. These usually occur from a twisting injury or a blow to the side of the knee that causes the meniscus to be pushed against and compressed.
Degenerative meniscal tears are best thought of as a failure of the meniscus over time. The meniscus becomes less elastic and complaint, and as a result may fail with only minimal trauma. It may be that there was no injury leading to the tear at all.
When you tear the meniscus, you may feel a "popping" sensation. This may or may not prevent you from continuing the activity you were doing. As the inflammation sets in, a number of symptoms and signs may present:
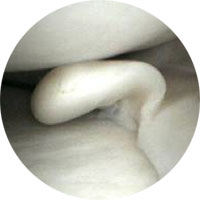
Figure 1: unstable tear of the meniscus on the inner side of the knee
The pain often improves with rest following the initial injury however the pain commonly recurs with twisting, squatting or aggressive activity. Joint swelling may occur although meniscal tears by themselves don't usually cause a tensely swollen knee. It may become difficult to fully straighten the knee (locking). This happens when a torn piece of meniscus displaces and becomes lodged in the hinge mechanism of the knee. If you think you have a torn meniscus, you should contact your local doctor as soon as possible.
You will be asked a detailed series of questions by your surgeon particularly how the problem started and what issues it is causing now. An examination will then be performed. Generally you will require an X-ray of the knee to look for any arthritis (wear and tear) which might also be causing your symptoms. Quite often you will be sent for an MRI scan to have a more detailed look at the knee.
Initial treatment for a torn meniscus is usually aimed at reducing the pain and swelling in the knee. You may be referred for physiotherapy to work on improving the range of movement and alleviate the pain and swelling. If you have a “locked knee” which cannot be straightened, surgery may be recommended as a matter of urgency to remove the torn piece of cartilage that is trapped in the joint. If your meniscal tear fails to heal on its own and your knee continues to be stiff and sore, surgery will be required to either remove the torn portion of the meniscus (partial meniscectomy) or to repair the tear (meniscal repair).
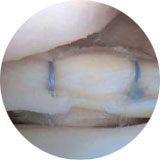
Figure 2 : meniscus on the outer side of the knee following repair with stitches.
Meniscal surgery is performed using an arthroscope (camera). A small incision is made in the knee to allow the insertion of the arthroscope into the joint. Through another small incision, special instruments are used to repair the meniscus while the arthroscope is used to see what is happening. Stitches are inserted into the torn meniscus until the tear is repaired (see fig 2). The success of the repair depends on a number of factors including the type of tear, the time from injury, your age and whether you have also injured your ACL.
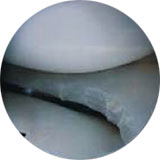
Figure 3: meniscus on the inner side of the knee after partial meniscectomy.
If the meniscus is not repairable, the torn edges will be trimmed off (see fig 3). This is commonly the case with degenerate tears seen in older people.
As with any operation, if something seems amiss it is better to get in touch rather than wait and worry.
These are very rare complications, however, the combination of knee injury, immobilisation of the limb, smoking and the oral contraceptive pill or hormonal replacement therapy (HRT) all multiply to make the risk greater. You should inform the surgeon if you have any history of thrombosis. Smoking should be stopped a minimum of one week prior to surgery.
This is more common in patients taking aspirin or nonsteroidal anti-inflammatory drugs NSAIDs) - such as naproxyn, voltarol and ibuprofen. These should be stopped at least one week prior to surgery.
Surgery is undertaken in an operating theatre in an ultra clean environment. Despite these measures, infection can still occur. This may present with a feeling of warmth and redness around the knee. It is imperative that this is not treated with antibiotics until you have seen your surgeon. Prolonged courses of antibiotics and / or further operations may be required and the recovery period will be delayed.
It is very common to develop a patch of numbness around your wounds. This is nothing to worry about and tends to shrink in size over time.
It is very common to experience pain around the scars. This may take up to a year to settle down.
A. General anaesthetic
A. Approximately 30-60 minutes.
A. Yes, unless advised otherwise.
A. Yes.
A. Yes, if you have had a meniscal repair. No, if you have had a partial meniscectomy.
A. Physiotherapy is commenced immediately. Your physiotherapist will supervise strengthening and walking.
A. Any blood thinning medication and hormonal preparations (such as the oral contraceptive pill) should be stopped. Your surgeon will inform you when the medication needs to be stopped
A. Driving an automatic car is possible as soon as pain allows after left knee surgery. If your right knee has been operated upon, driving is allowed when you can walk independently and can make an emergency stop.
A. This usually settles within 2-4 weeks of the operation.
A. Sedentary and office workers may return to work approximately 2-5 days postoperatively.