Total Knee Replacement
If you have further questions about total knee replacement then please feel free to contact us
here.
Alternatively you can book an appointment to see us below.
Osteoarthritis is a very common condition which affects the body's joints. The articular cartilage (gristle) lining the ends of the bones becomes worn and the joint no longer moves as smoothly as it should. The knee joint is the most common large weight bearing joint to be affected.
There are a number of factors which can increase the risk of osteoarthritis. Very often these factors combine and lead to the condition. Osteoarthritis is twice as common in females as it is in males. It is more common the older we get (over the age of 40) and is clearly linked to obesity and also previous joint injury. There is a strong genetic component to knee osteoarthritis and the condition tends to run in families. Very often however, there is no clear cause for osteoarthritis - it just happens.
Pain and stiffness are the most common symptoms. This pain tends to be worse with movement of the joint or at the end of the day. Stiffness is classically worse after a period of inactivity or rest but walking tends to ease the stiffness within a few minutes. The joint may creak or grind as you move and may also become swollen.
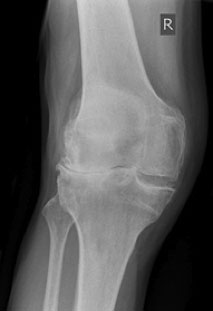
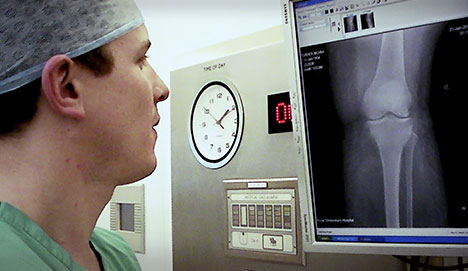
Figure 1: X-ray of the right knee showing the typical features of osteoarthritis, joint space narrowing and spurs of bone
There is no blood test to diagnose osteoarthritis. The diagnosis is readily made on symptoms and clinical signs on examination. X-rays are used widely to confirm the diagnosis. An x-ray is likely to show narrowing of the space between the bones where the gristle has worn and also spurs of bone.
Occasionally, an MRI (magnetic resonance imaging) scan will be undertaken to look at the extent of the arthritis and the state of the soft tissues (shock absorber cartilages, gristle, and ligaments) which are not readily seen on an x-ray.
This can be broadly classified into conservative (non-operative) and surgical. The mainstay of initial treatment is conservative. It is important to keep the affected joint mobile and the muscles acting upon them strong. For this reason, regular low-impact exercise and physiotherapy are first-line treatments. In addition, regular painkillers (e.g. paracetamol) and anti-inflammatory medication (e.g. ibuprofen, naproxen) are used to control symptoms. If you are overweight, the single most important factor in improving symptoms is weight loss.
Other conservative treatments include steroid injections which may provide short term relief of symptoms.
Total knee replacement should be considered when you have severe osteoarthritis and your symptoms are no longer controlled with conservative measures such as pain killers, weight loss and injections. When these symptoms severely affect the quality of your life and restrict your ability to undertake activities of daily living, surgery may be indicated. The decision to proceed with TKR should be made by you but should involve input from your surgeon and also your family.
TKR is a major operation and its success relies on dedicated rehabilitation after the operation. The operation will relieve your arthritic pain, but you will be left with a different type of pain from the procedure itself as a result of cutting soft tissues and bone. It may take up to a year for the knee to settle down and for you to realise the benefit of the procedure.
You will be seen in the preadmission clinic before your operation. You must inform your doctor of any relevant medical history such as diabetes, blood clots, heart problems, any associated medication such as blood thinning medication (e.g. warfarin or clopidogrel) which will need to be stopped prior surgery) and any drug allergies.
Generally, you will be admitted to hospital on the day of your operation. In some cases you will be admitted the night before. It is very important that you contact your surgeon if you have any spots, ulcers or broken skin around the area to be operated on OR if you are unwell with a cough, cold or other infection.
The consultant anaesthetist looking after you will discuss the options available. Most patients will have a general anaesthetic which is often combined with a spinal (injection in your back) or local anaesthetic nerve blocks. Your surgeon will inject local anaesthetic around the knee joint throughout the procedure to try to minimise pain during and after the operation.

The procedure normally lasts 1-2 hours and involves a 20cm incision (approximately) made over the front of the knee. The worn out surfaces at the end of the thigh and shin bones are cut away using special instruments. If the back of the kneecap is badly worn, then this worn part will also be removed. The bony surfaces of the thigh and shin bone are then replaced with tough metal implants, generally made of cobalt chrome, while the back of the knee cap and the spacer between the metal implants are made of tough plastic (polyethylene). Once the components are cemented in place the knee is closed with sutures and clips. Occasionally, a drain will be left in your knee which will be removed after 24 hours.
You will be given foot-pumps (to increase blood flow away from your legs) and blood thinning injections to prevent blood clots. The foot-pumps will be used until you are mobile, while the injections will start the day after the operation and continue for 10 days after the operation. You will be mobilised by the physiotherapists as soon as possible after the operation. This is beneficial in preventing blood clots and preventing chest infections. Following the operation, you are likely to be in hospital for 3-5 days. You will be discharged with crutches which you will need to use for a few weeks until you are confident walking unaided.
Fortunately the risk of complications following total knee replacement is low. If you are unfortunate enough to develop a complication, it may delay your recovery and impair your overall long-term outcome.
Deep infection: the overall incidence of deep infection is approximately 1%. Its treatment may involve prolonged courses of antibiotics, and further operations.
Damage to the nerves and /or vessels behind the knee is rare.
Blood clots: about 1 in 10 patients will develop a blood clot in the calf which causes them symptoms, while about 1 in 100 patients will develop a blood clot in their lungs (embolus). The incidence of death following an embolus is 1 in 3000.
The incidence of death from all causes in the first 3 months after total knee replacement is 1 in 200.
Stiffness: the knee is usually quite stiff for up to 3 months. 1-2% of patients following total knee replacement will develop stiffness that needs treatment. The average range of motion following a total knee replacement can be expected to be 115°.
Numbness: it is extremely common to notice numbness around the wound. This may improve with time.
Wear and Loosening: the components may wear out in your lifetime; 90% of total knee replacements will last 10-15 years.
Persistent pain: 10-15% of patients will experience continuing pain following total knee replacement; very often this will be unexplained.
Fracture: if you were to have a heavy fall, you could fracture (break) the bones around the knee and your knee replacement could loosen.
A. Yes, this is an essential part of recovery. This can be as an inpatient or an outpatient. The physiotherapy is organised after your operation by the hospital staff.
A. Avoid for 6 weeks after a RIGHT total knee replacement. Avoid for 2 weeks after a LEFT total knee replacement (when driving an automatic car).
A. It can take 3-6 months before the size of the knee returns to normal. The knee may also feel slightly warm for this period.
A. 90% of total knee replacements will last for 10-15 years before showing signs of wear and loosening.
A. The metal component is made from cobalt chrome and the liner from high density polyethylene.
A. This depends very much on your occupation. If you’re job involves light duties (office based) it would be possible to return to work within 2-4 weeks. If your job involved heavier activities, work could be resumed between 2-3 months after surgery.
A. The hospital will provide you with stockings following your total knee replacement surgery. The stockings are required to remain on during the day for 6 weeks post surgery. The stockings can be taken off at night.
A. Owing to a combination of a tender scar and a lack of knee bend, only 1 in 3 patients will be able to kneel after knee replacement.
A. Impact activities such as running should generally be avoided because of the risk of prematurely wearing out the implant. Activities such as walking, sailing, bowls, doubles tennis, swimming, cycling and golf are encouraged and should be possible from 2 months postoperatively.